Becky Larson
In 1992, Becky Larson was a young mother of three, looking for a job that allowed her to work remotely. Because options for virtual work were limited at the time, she found herself in the world of medical transcription, which ultimately led her to a variety of roles in medical simulation. She quickly became passionate about the work and the technology’s ability to allow students to practice their skills in a safe environment. Today, Larson is the simulation specialist at Surgical Science, which manufactures and develops laparoscopic virtual reality simulation devices. In this Q&A, learn about her experience with virtual surgical simulation, what program directors are saying about the technology, how the CARES Act can help programs access it, and more.
When it comes to simulation, and virtual simulation in particular, what changes have you observed over the course of your career? How far has the industry come and what is on the horizon?
When I started in the medical simulation industry in 1999, it was just in its infancy and many people did not understand what it was. There were just a few companies out there and we really needed to prove the value of simulation training. With the help of institutions doing research, we have come a long way. The technology behind virtual reality (VR) simulation has made significant progress in the last few decades, thanks to key improvements to anatomy and data feedback that make it more effective than traditional methods and box trainers. The anatomy now looks and feels so lifelike and provides a very realistic and safe environment to practice without risk to the patient. For the educator, VR simulation reduces the demands on supervision and leads to more skilled students that are ready for the OR. I am very excited about what is next to come. I believe we will be able to replicate a patient’s existing condition or pathology, add it to the simulator, and practice using the patient’s replicate before operating.

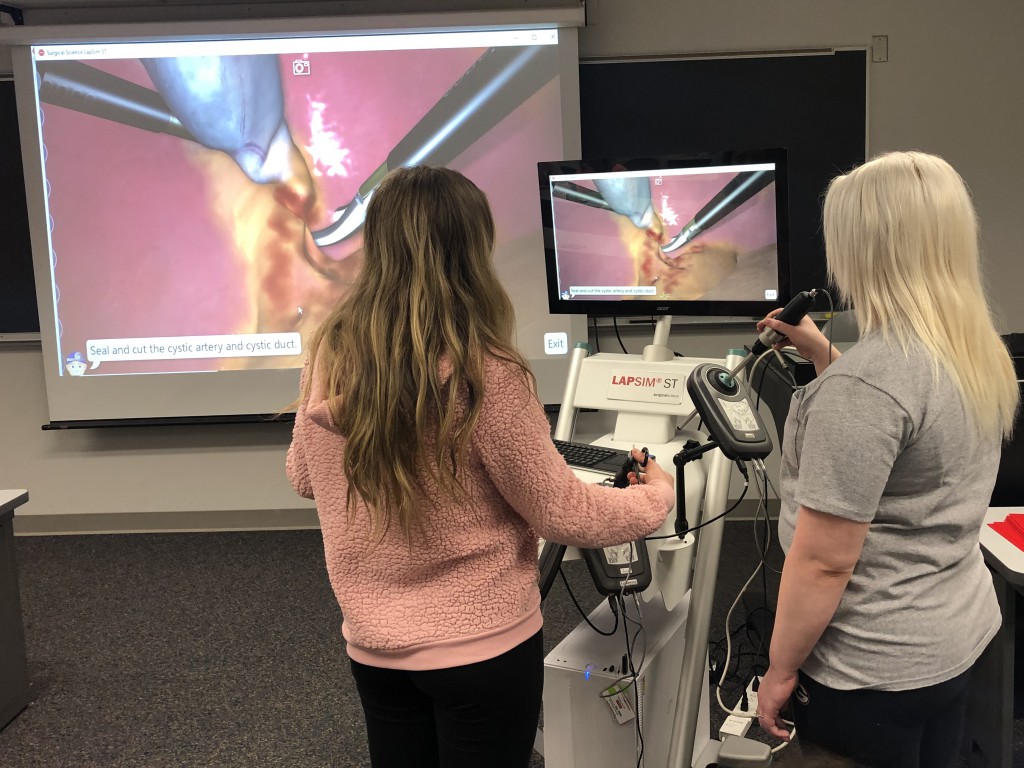
A look at Larson’s past visits with surgical technology and surgical assisting students as they try their hand at virtual simulation.
What is the value of virtual simulation, especially when many surgical technology and surgical assisting students and instructors are seeking remote learning options?
The greatest value is that a student gains a high level of competency before they step into the OR. With the pandemic, getting students into clinicals is challenging, which means less practice time. My customers are telling me that they need this now more than ever. VR simulation can be accessed 24/7 when it’s in the lab; however, now that our company has added a portable kit, both the educator and the student have the ability to learn and polish their practical skills as their schedules allow. Program directors and instructors can also use the simulator for a Zoom class and share their screen while they are navigating the camera in a virtual anatomical environment.
What kind of anecdotal feedback have you received from program directors and instructors who utilize this technology? Do they find it beneficial and if so, how?
Program directors and instructors quite often share they are grateful for this technology and that it has made their lives easier. They find it provides a realistic, hands-on experience that prepares their students for the OR. After a student does an exercise, they receive immediate, objective feedback, which provides reinforcement for skills development. Practicing in a safe environment builds confidence, and the program directors are getting positive comments about their students’ performance at clinicals. Directors love that they can use it at recruiting events because it attracts new students to their program, too.
Can you share more information about the Coronavirus Aid, Relief and Economic Security (CARES) Act and how you’re seeing schools obtain funding for their labs through it?
Because the CARES Act supports the costs of shifting classes to online learning, many program directors, with the help of their deans and administration, have been able justify purchasing this equipment. Some program directors and instructors were not aware their school had access to these funds. Because virtual reality simulation will help the surgical technology and surgical assisting programs transition to a more compelling hybrid program, it can justify the need for CARES Act funding. It is a very small silver lining amid this pandemic. In more than 20 years of working in medical simulation, I am confident that this technology is one essential way to keep patients safe. Programs should explore the technology based upon their budgets and take advantage of the CARES Act, the Carl D. Perkins Career and Technical Education Act of 2006 (Perkins IV) or other grants available to finance these game-changing tools. There are a ton of resources out there, and many schools have grant writers available to help program directors obtain what they need to help their students succeed.
The resources shared in this article are intended for information-sharing purposes only. Sharing of this information does not indicate promotional endorsement from ARC/STSA.
