Featuring Anthony J. LaPorta, MD, FACS, Director, Military Medicine Program at Rocky Vista University and Kit Lavell, BA, Executive Vice President at Strategic Operations
From virtual simulation to synthetic cadavers and more, surgical technology and surgical assisting programs are incorporating the very latest in innovative, hands-on training activities into their curricula. The Cut Suit is a simulation tool that is worn by a live human and replicates the look and feel of traumatic injuries.
Designed by surgeons for surgeons, the Cut Suit allows students to practice for high-pressure situations with room to safely make non-life threatening errors. Anthony LaPorta is the director of the Military Medicine Program at Rocky Vista University in Colorado, and has used the Cut Suit with students for the last 10 years. “We’ve trained hundreds of medical students using the technology, and the results are consistently astounding. The suits are very reusable [and] very versatile.” As a respected expert in the field of military medicine, LaPorta was involved in the development of the Cut Suit but does not have an economic stake in the resource.
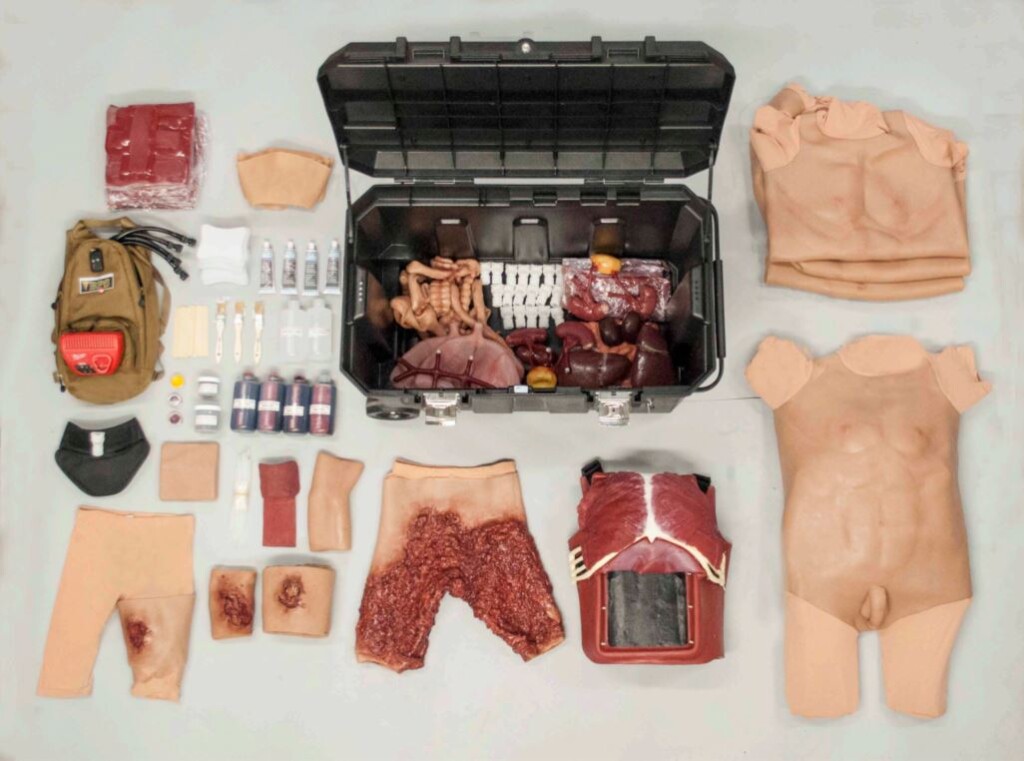
Pictured above is the Cut Suit and its multiple components. The suit is intended to be worn by live patient “actors” and helps simulate trauma events.
Kit Lavell, executive vice president at Strategic Operations, which produces Cut Suit, explains that the realistic simulator accounts for the various pitfalls and the complications that could be encountered in each procedure, offering the benefits of live patient training without ethical or practical issues. For example, “time out” can be taken for instruction and education. “Mistakes can be made and taken to a point where true learning of how to recover from the mistake can be experienced safely,” Lavell explains.
LaPorta notes that Cut Suit training has led to dramatic improvements in students’ technical skills and their ability to identify surgical instruments. He relates his experience with Cut Suit training to his time as a military surgeon.
“This is how we train students in the military,” LaPorta says. “You have to let students make mistakes in real-time and learn from them. The Cut Suit offers the benefits of habituation training in a controlled setting.”
While the Military Medicine Program at Rocky Vista University largely works in training students to become physicians, this simulator also provides many benefits for surgical technology and surgical assisting students. The Cut Suit can be used in collaboration with other programs for trauma training, wherein EMS students stabilize the patient, nursing students triage the patients, radiology students prepare for imaging, and surgical technology and surgical assisting students prepare the operating room and assist with surgery.
The Cut Suit also helps to humanize the patient, ultimately allowing surgical technology and surgical assisting students to build soft skills around patient management. Because the suit is worn by a live human, students get a feel for treating a person rather than an inanimate object. The patient actor can express themselves freely — screaming, panicking or fighting — which makes for a realistic learning experience that students can’t ignore in the moment.
As it becomes more common to perform some surgeries without general anesthesia — for example, orthopedic procedures that use spinal anesthesia, C-sections where the patient is awake and some traumatic scenarios where patient is brought in awake — learning how to engage with and soothe a patient in high-stress environments early on will only empower surgical technologists and surgical assistants in their learning journey. The Cut Suit is just one option among many simulation tools that help students become increasingly familiar with their role in the operating room — and most importantly, care for the safety and well-being of the patient.


Anthony LaPorta, MD, FACS (left), is a professor of surgery and the director of the Military Science Program at Rocky Vista Mountain University in Parker, Colorado. LaPorta retired from the U.S. Army as a Colonel after over 26 years of service. He has authored more than 200 peer-reviewed articles and presentations on surgery, immunology, military medicine, and simulation. He originally trained in surgery at the Medical College of Wisconsin and the University of Oxford, England.
Kit Lavell, BA (above, right), is the executive vice president of Strategic Operations. In the past 18 years, he has helped the company grow to provide training support for U.S. military operations to more than 950,000 military and civilian first responders. Lavell is a graduate of the University of Illinois, has done graduate work at California State University Fresno and attended the Naval Postgraduate School.
Disclaimer: The resources in this article are shared for informational purposes and not intended as a promotion or product endorsement by the ARC/STSA.
